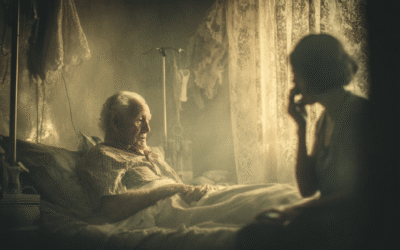For some aged care residents, holding a doll brings comfort. For others—especially staff or families looking on—it can raise eyebrows. But beneath this gentle act lies a powerful and surprisingly effective therapy: one that’s calming distressed residents, improving communication, and offering connection where words and memory have faded. Known as doll therapy or child representation therapy, this approach is being embraced in more Australian aged care homes—not without controversy, but often with heartening results.
What Is Doll Therapy?
Doll therapy involves giving a lifelike doll to a person with dementia, often someone who was once a parent or caregiver. The idea isn’t to play make-believe, but to meet the person in the emotional world they’re living in now.
For someone with dementia, especially in the later stages, abstract reasoning and short-term memory often fade. What remains strong are emotional memories—particularly those linked to attachment and caregiving. Holding a doll can tap into these deeply rooted instincts, giving a sense of purpose and calming restlessness.
As dementia support specialist Dr. Eva Kittay puts it, “The therapy doesn’t ask a person to leave their reality. Instead, it joins them there—with gentleness and respect.”
The Evidence: What Research Shows
Growing research backs up what many carers see anecdotally: doll therapy works—when introduced with care.
- A 2021 Italian randomised controlled trial found that residents given dolls showed significantly reduced agitation, apathy, and wandering compared to those receiving usual care.
- A 2024 scoping review published in Dementia & Geriatric Cognitive Disorders concluded that doll therapy improves mood, encourages communication, and reduces distressing behaviours across multiple settings.
- Observational studies have noted positive impacts on nutrition and daily routine—with some residents becoming calmer and more engaged during mealtimes when holding their doll.
Locally, aged care providers like Mayflower and Arcare report similar outcomes. “We’ve seen non-verbal residents begin talking to their dolls, smiling more, even eating better,” one Mayflower staff member told ABC News in a 2023 segment.
Doll Therapy in Australia
Doll therapy is increasingly used across Australia, though practices vary widely. In many aged care homes, it’s part of diversional therapy programs—non-medical approaches that aim to stimulate wellbeing through meaningful activity.
Dementia Support Australia (DSA) and the Aged Care Research & Industry Innovation Australia (ARIIA) both include doll therapy in their resources for managing behavioural and psychological symptoms of dementia (BPSD). Their guidance emphasises the importance of care plans, consent, and ongoing review.
One regional example is the program run by Play Move Improve, an Australian occupational therapy service working with rural care homes. Their founder, Leanne Bell, says empathy dolls are “gentle tools that often unlock emotion when nothing else does.”
Yet implementation is patchy. Some care homes embrace the approach; others remain cautious or avoid it entirely. Concerns about infantilisation and staff discomfort are common barriers—more on that below.
Dos and Don’ts: What Makes It Work?
The difference between successful doll therapy and a distressing experience often comes down to how it’s introduced.
DO:
- Obtain consent where possible—from the resident or next of kin—and document it in the care plan.
- Respect the emotional reality of the person. If they call the doll “my baby,” follow their lead. Don’t correct or contradict.
- Use lifelike, diverse dolls with soft features. Dolls with open eyes, weight, and realistic clothing tend to be more effective.
- Treat the doll with care. Mishandling or “taking away” the doll can be traumatic.
- Monitor outcomes: Is the resident calmer? Are they sleeping better, eating more, or communicating more?
DON’T:
- Force the doll on anyone. If the person isn’t interested, that’s okay.
- Use dolls with closed eyes or sound effects, which can be confusing or distressing.
- Talk down to the resident or use patronising language. This isn’t about pretending they’re a child—it’s about meeting them emotionally.
- Allow staff to use dolls as “tools of compliance” or to quiet someone down without further engagement.
A Question of Dignity
The ethical debate around doll therapy often centres on dignity. Is it infantilising? Are we fooling residents into a false sense of reality?
There’s no simple answer. Critics argue that giving a doll to an adult strips away autonomy and treats them like a child. Others worry it can lead to obsessive attachment or conflict if dolls go missing or are taken by others.
But supporters say the opposite: that doll therapy, when offered with respect and choice, honours a resident’s reality and offers comfort no drug can match.
As one aged care nurse from Victoria’s Gippsland region put it, “We’re not pretending they’re children. We’re honouring their need to love and be needed.”
There have been rare but serious breaches. In 2022, a therapist in a NSW facility was reported for deliberately mistreating a resident’s doll as a form of punishment—an act the Health Care Complaints Commission labelled “callous and degrading.” This case has since been used as a training example for why empathy, supervision, and ethical boundaries matter.
Choosing the Right Doll
The doll’s design plays a crucial role. It should:
- Be soft-bodied and realistic, with gentle features
- Have open eyes and human proportions
- Reflect diverse ethnicities if possible
- Be washable and safe for hugging or rocking
Some facilities use weighted dolls for added comfort. Others keep a collection so residents can choose, reducing attachment conflicts.
Importantly, the doll should be treated like a real object of affection—not a prop to be tossed aside. Staff should be trained to handle dolls gently and avoid scenarios where dolls are “confiscated” or dismissed.
Training and Policy
Implementing doll therapy responsibly requires:
- Staff training in emotional intelligence, dementia communication, and ethical use
- Written policies that cover consent, monitoring, and removal protocols
- Ongoing review: not all residents will benefit, and needs can change over time
- Family engagement to reduce misunderstandings and offer reassurance
As part of a broader dementia care strategy—including music therapy, sensory gardens, and life story work—doll therapy can slot in as one of many non-pharmacological tools.
Regional Realities
In regional and rural care homes, where access to specialist dementia services may be limited, doll therapy offers a low-cost, high-impact option. Weighted empathy dolls range from $60 to $150 and don’t require ongoing technology or internet access.
For smaller homes with limited budgets and staffing, doll therapy can bridge a gap: calming agitated residents, easing meal routines, or simply offering moments of connection when time is short.
In Victoria’s South Gippsland, one rural facility trialled doll therapy after seeing a spike in anxiety among residents with dementia. Staff reported fewer after-hours calls and improved sleep among participants.
Looking Ahead
Doll therapy isn’t a miracle—but it is a meaningful, evidence-backed approach that speaks to something deeply human: the need to love and be needed. When implemented with dignity, empathy, and careful planning, it can bring calm to chaos and presence to people often lost in fog.
In Australia, there’s growing interest in combining doll therapy with other innovations—from sensory rooms to robotic pets. But no matter how sophisticated the tools become, the core remains the same: connection.
And in aged care, connection is everything.