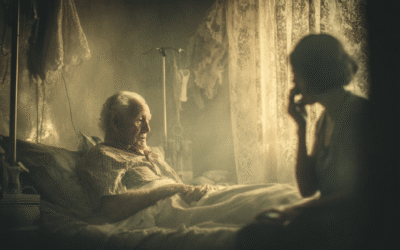TL;DR
Australia’s sandwich generation, those caring for both young children and aging parents, face escalating pressure not just from emotional or financial load, but from fragmented service systems. This article explores how the lack of integration between My Aged Care, NDIS, and childcare funding creates a hidden third job for carers: navigating bureaucracies that don’t speak to each other. It calls for policy reform to streamline access, reduce duplication, and recognise carers as central, not incidental, participants in service delivery.
Many working Australians are quietly doing three jobs. The first pays the bills. The second is raising children. And the third, largely invisible, unpaid, and unrelenting, is caring for an aging parent.
This is the reality for the sandwich generation: the adults caught between two sets of dependents, with little time, energy, or income left for themselves. It’s a growing demographic, mostly women aged 35 to 64, doing what the aged care and childcare systems can’t.
But the true weight of this double-duty life isn’t just emotional or financial. It’s systemic.
What’s breaking people isn’t the love they feel or the time they give. It’s the bureaucracy. Three major care systems, NDIS, My Aged Care, and Childcare Subsidy, were designed to function independently. But for carers juggling all three, it feels like managing parallel universes: different logins, lingo, eligibility rules, and hours of unpaid administration.
This article explores how fragmented systems deepen the care squeeze, and why policy integration, not just personal resilience, is the reform we desperately need.
1. Three Systems, One Carer
If you’re raising a child, supporting a parent with dementia, and helping a teenager with a disability, all while trying to hold down a job, you’re not dealing with one care system. You’re dealing with three.
Each of Australia’s major care pillars, My Aged Care, the National Disability Insurance Scheme (NDIS), and the Child Care Subsidy (CCS), operates as its own bureaucratic universe. Each has its own language, eligibility criteria, funding models, and points of access. None are built to recognise a carer’s full picture.
Let’s break it down:
- My Aged Care focuses on over-65s needing help at home or in aged care facilities. It requires formal assessments, approved providers, and service coordination that often assumes a carer is present and able to fill in the gaps.
- NDIS supports people under 65 with permanent disabilities. The funding can be life-changing, but it demands intensive paperwork, annual reviews, and careful budget management. Many parents find themselves becoming part-time plan managers just to keep their child’s support stable.
- Child Care Subsidy is designed to help working parents access early learning. But its rules assume standard employment patterns and often ignore the irregular demands placed on carers who are also juggling aged care or disability needs.
Now imagine one carer navigating all three simultaneously.
There’s no shared intake. No linked data. No recognition across systems that a person might be both a mother, a daughter, and a disability support coordinator at once. Instead, each role must be performed separately, and the burden of integration falls not on the system, but on the individual.
It’s not just exhausting. It’s inefficient. And for thousands of families, it’s the silent source of their burnout.
2. The Invisible Labour of Navigation
For sandwich carers, the hardest part of the job often isn’t the care itself. It’s the admin.
Applications. Assessments. Phone queues. Repeat documentation. Service plans. Funding reviews. Conflict resolution. Chasing emails. Waiting on hold. Explaining the same story to a new case manager every six months. It’s not dramatic, but it’s relentless.
This hidden load is what many carers describe as a “third shift”, not childcare, not elder care, but system care. It requires the skills of a project manager, advocate, translator, and sometimes even a lawyer. And it’s almost always unpaid.
“I spend more time filling out forms than I do spending time with my kids,” says Melissa, a 42-year-old sole parent caring for her autistic son and elderly mother. “Every service wants something different, Medicare numbers, bank statements, NDIS goals, proof of income. I feel like I’m working for them, not the other way around.”
There’s data to back her up. According to Carers Australia, many unpaid carers spend over 15 hours a week coordinating care, on top of direct caring responsibilities. For those navigating multiple systems, that number can double. Yet none of this time is counted in official productivity stats. It doesn’t register in GDP. And it certainly doesn’t earn super.
This work is often invisible even to close friends and employers. Because it doesn’t involve uniforms or hospital visits, it’s easy to overlook. But the psychological toll is real: decision fatigue, chronic stress, sleep disruption, and a loss of identity outside the role of “carer.”
System navigation also becomes a barrier to equity. Families with lower digital literacy, limited English, or poor internet access are disproportionately disadvantaged. And carers in rural or regional areas may find the nearest support coordinator is hundreds of kilometres away.
In short, this unpaid navigation is a silent cost, a tax paid in time, stress, and missed opportunities. And yet, it’s the glue holding Australia’s fragmented care architecture together.
3. When Systems Collide
When you’re navigating three different care systems, it’s not just the paperwork that multiplies, it’s the contradictions.
Take Angela, a mother of three in outer Melbourne. Her youngest son receives early intervention through the NDIS. Her father, recently diagnosed with Parkinson’s, has a home care package through My Aged Care. But when Angela tried to coordinate respite care for both, on the same day, through the same provider, she hit a wall.
“They told me they couldn’t combine services across funding streams. I had to book two separate workers, through two different departments, and fill out two sets of reports,” she said. “It was ridiculous. We’re one family.”
These service silos create policy frictions that make life harder, not easier:
- My Aged Care doesn’t recognise NDIS-funded carers within the same household for scheduling or cost-sharing.
- Child Care Subsidy assumes parents are working standard hours, not flexible, casual, or part-time carers balancing medical appointments and aged care visits.
- NDIS planners may not factor in the needs of other dependents when setting a support budget, leaving parents to triage care based on what’s fundable, not what’s necessary.
These aren’t edge cases. They’re everyday realities for families who don’t fit neatly into the boxes bureaucracies are built on.
The impact is especially sharp in rural and regional Australia, where services are already thin on the ground. And culturally diverse families may face added hurdles with system literacy, translation, or differing understandings of what “formal” care even looks like.
When systems collide, carers don’t just fall through the cracks, they spend their days patching the cracks themselves.
4. Better Models Already Exist
The care squeeze may feel inevitable, but it isn’t unsolvable. Around the world, and even in pockets of Australia, better models already exist.
In Finland and Sweden, for instance, integrated family service centres offer a one-stop hub where parents can access childcare, elder care advice, disability support, mental health services, and financial counselling, all under one roof. Staff are cross-trained, records are shared, and the system is designed to reflect family life, not administrative convenience.
“They don’t ask who you’re caring for,” said one Australian social policy researcher. “They ask, ‘What do you need today?’ That simple shift in approach changes everything.”
Closer to home, several Aboriginal-controlled health organisations in Australia already offer this kind of wraparound support. By combining early childhood education, elder support, community health, and family violence services in culturally safe environments, they provide a living example of what joined-up care can look like. Families don’t need to re-tell their story to five different case workers, they build relationships over time, with people who see the whole picture.
There are also pilot projects underway. In regional Victoria, a trial community navigator program brought together local councils, hospitals, and family services to provide carers with a single point of contact. Feedback was overwhelmingly positive, but the funding was time-limited, and the program now faces an uncertain future.
What these examples show is that system integration isn’t a fantasy, it’s a design choice. With the right political will, funding, and structural support, Australia could move toward a model where care systems collaborate instead of compete.
Because no one should need to be a full-time bureaucrat just to love their family.
5. What Needs to Change
Fixing the care squeeze isn’t just about more funding, it’s about smarter, more connected systems that treat carers as central, not incidental.
Here’s what experts and carers themselves say needs to happen:
- Unified Intake and Navigation Tools
Develop a single digital entry point that allows carers to register needs across aged care, disability, and childcare. Much like MyGov, but designed around families rather than individuals.
- Shared Care Plans
Create care plans that travel with the person and family, recognised by multiple agencies. This would avoid duplicate assessments and reduce the burden on carers to explain everything again and again.
- Funded Care Navigators
Introduce a Medicare-funded care navigator role, available through GPs or local councils. These workers could guide carers through the maze, connect services, and advocate across systems.
- Cross-System Training for Staff
Ensure frontline workers understand all three major care systems, not just their own. This could help spot overlaps, gaps, or red flags before families hit crisis point.
- Carer-Centric Policy Design
Involve carers in policymaking from the outset, not as an afterthought. Recognise that many policies still assume a carer only has one person to support.
These changes won’t happen overnight. But they are feasible, and they reflect what’s already working in small-scale trials.
Carers aren’t asking for luxury. They’re asking for logic, compassion, and systems that see the full picture.
Australia’s sandwich generation isn’t breaking because they care too much. They’re breaking because our systems expect them to carry the weight of disconnection.
The burden of navigating aged care, NDIS, and childcare as three separate worlds doesn’t just cost time, it costs health, income, relationships, and often the very quality of care we claim to prioritise. Behind every government portal or assessment form is a human being trying to keep multiple generations afloat, often without rest or recognition.
It doesn’t have to be this way.
Integrated care isn’t a radical idea, it’s a practical one. It’s already happening in Aboriginal health centres, Scandinavian family hubs, and small community-led pilots around Australia. What’s missing is scale, consistency, and political courage.
If we want to support carers, we need to stop treating them like shadows behind the people they care for. They are decision-makers. Navigators. Often, the glue that holds failing systems together.
And if we’re serious about fixing the care crisis in this country, we have to start by seeing the whole family, not just the funding stream.
Because no system is truly caring until it cares for the carer, too.